Healthcare is moving inextricably toward a more connected future, with clinicians using data that crosses boundaries between devices and systems to offer insights for holistic, precision-based care. Increasingly, providers are seeking to improve care with digital technology that connects the dots of previously siloed healthcare data and moves them from episodic, and largely reactive care to proactive, preventive care intended to head off adverse events before they happen.
As this year’s Philips Future Health Index report reveals, healthcare leaders are becoming ever-more confident in the importance of connected data in driving smarter clinical decisions and encouraging greater operational efficiency. The 2022 report showed that nearly two-thirds (65%) of healthcare leaders believe that the value data brings to areas such as digital health records, patient monitoring and medical devices makes the time and resource investments required worthwhile.[1]
Further, the report showed that healthcare leaders see tremendous value in the predictive analytics that can come from having integrated, contextualized medical device data:
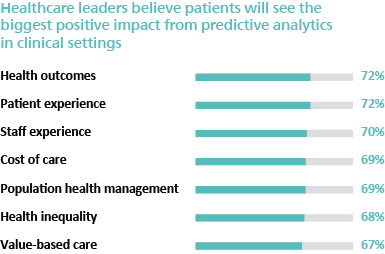
But at the same time, just over half (51%) of respondents in the report said that data siloes hinder their ability to use data effectively across clinical and operational workflows. They cited limitations in their technical infrastructure, data security and privacy, and staff knowledge as key data challenges.
Further, in many instances, existing hospital technology systems may not be able to capture all the data that’s streaming from their medical devices, or fail to deliver captured data to systems of record in a way that’s useful to clinicians. In fact, in a 2019 article, the World Economic Forum reported that 97 percent of data produced by hospitals each year – from tests, clinical notes, imaging, sensors, etc., – goes unused.[2]
How do health systems overcome these data obstacles?
Medical device integration (MDI) technology, supported by a data management system and an IT infrastructure for sharing information, is at the heart of liberating data from disparate medical devices, aggregating and analyzing the data, and sharing insights – in context to the patient – with the care team. For a successful medical device integration strategy, I would focus on a technology platform with the following key capabilities: centralized management, scalability, and security.
It stands to reason that a technology platform for integrating medical device data should be easy to implement and support, and provide visibility for all the hubs, device and gateway connections, and application configurations that are part of the system.
With the visibility of centralized management, system administrators can remotely see the medical devices connected to a device integration platform and all the data flowing in and out. This makes troubleshooting and system diagnostics easier, as systems administrators will be able to quickly spot clinical components that aren’t sending data and need maintenance.
Importantly, centralized management gives MDI systems the ability to configure which data points are sent out to different downstream systems, such as EMRs, decision support applications or research databases. So much data streams from hospital medical devices – patient numeric vitals and waveforms, and clinical alarms – that being able to easily capture and direct that data, in a timely fashion, to specific downstream sources plays a significant role in supporting care delivery and enhancing productivity.
Centralized management also provides a simple way to make data that’s received more relevant, by refining and tailoring it so that so that clinicians receive the data that’s most important to them, when they need it.
Selecting a device integration platform that is scalable will make it easier to adapt as hospitals add medical devices and expand their use of data. Scalability gives an MDI system the flexibility, security, and reliability to manage simple and complex deployments of new devices throughout the hospital or from additional facilities or departments that come online. This provides the reliable and timely delivery of medical device data, which is critical to supporting rapid change in health system procedures, creating insights for patient care, creating operational efficiencies, and supporting new care models.
Privacy and access control for an MDI system should include capabilities for secure, centralized mechanisms to manage the identity, authentication and authorization of users, services, and devices. It should also enable access control to provide privacy for sensitive data.
Key MDI capabilities that can enhance security include:
Capsule Medical Device Integration captures live streaming data across connected devices while simultaneously formatting and standardizing it to appear source-independent and consistent across devices and manufacturers to meet different clinical initiative use cases.
The newest release of the Philips Capsule Medical Device Information Platform includes the Philips Capsule Command Console (C3), a centralized management tool for administrative activities. C3 makes it easier to implement and support the Capsule MDIP. C3 provides single visibility and management of the Capsule MDIP, hubs, connections, and application configurations through a modern, web-based application. Enhanced controls and live remote views ease deployment and management by providing searching and filtering of connected hubs and access to hub details and status.
Christopher Cage is a Product Manager working on Product Management Platform & Integration at Capsule Technologies.
Learn more about Capsule Command Console, the centralized management tool of the Philips Capsule Medical Device Information Platform.
Download