Florence Nightingale, an English social reformer, statistician and the founder of modern nursing, wrote in 1859: “Unnecessary noise is the most cruel absence of care which can be inflicted either on sick or well.” [1]
Imagine what Nightingale would say if she were alive today!
Modern hospitals are awash in sound. Monitors, alarms, pumps and other equipment provide vital data to support clinical care, but also produce noise levels unheard of decades, let alone a century, ago.
One patient monitor in a typical, modern Intensive Care Unit (ICU) can produce between 200-400 alarms per patient, per day. Furthermore, most of these alarms are false or clinically insignificant, with 85–99% of all alarms being non-actionable. [2] Most hospital rooms house two patients separated by a curtain, which means each patient experiences a double whammy of beeps, buzzes and alarms.
All this noise negatively impacts patients, their families and the clinical staff.
There are many root causes for the proliferation of non-actionable and clinically insignificant alarms. [7]
Among the most common is poor skin preparation for electrocardiograms (EKGs), improper electrode placement and pulse oximetry finger probes that become dislodged and cause alarm “misfires.”
Also common is inadequate battery management, resulting in “low battery” alarms, as well as devices unable to send data to central stations.
Alarm system settings can contribute to the problem – lack of standardization for default settings, inconsistent use of system features and default system limits that are too tight or not personalized can trigger alarms that are not clinically actionable.
Training and policies play an important role when it comes to alarm system settings, with inadequate training in alarm management policies and protocols, or lack of best practices for customizing alarm systems to actionable limits for each patient leading to random or inconsistent alarms.
The perils of alarm mismanagement have caught industry and regulators’ attention.
To understand the root causes and bottlenecks and drive improvements, and more importantly, provide continuous measurements and monitoring to sustain those improvements, one must be able to establish a baseline of various metrics related to root causes of clinical alarms.
Philips Capsule Alarm Insights Manager (AIM) is a cloud-based solution that provides an interactive, intuitive set of alarm key performance indicators (KPIs) to assess alarm burden over hours, days, weeks, or months, by clinical unit, patient, alarm type or severity. These KPIs provide insights into root causes of alarms, thus arming our clinical consultants with evidence to establish recommendations and training with the goal of reducing non-actionable, nuisance and clinically irrelevant alarms.
Alarm Insights Manager also helps identify potentially actionable insights into hospital alarm system quality, with the aim of combating alarm fatigue and establishing best practices. It also allows benchmarking historically and across units for continuous improvement monitoring.
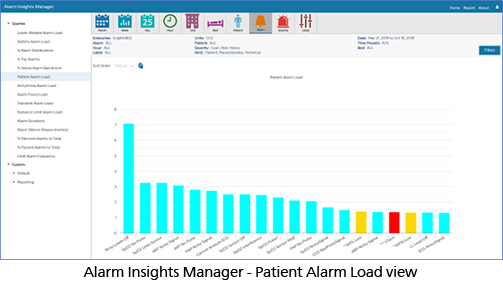
Philips Capsule’s Alarm Insights Manager supports healthcare’s quadruple aim in several ways.
By enabling a quieter and safer environment for the patient that promotes better sleep and less anxiety, Alarm Insights Manager can potentially enhance a patient’s healing process. Fewer nuisance alarms can mean less sensory and cognitive overload for clinicians, and less time responding to clinically irrelevant alarms, which can potentially allow for more focus on actionable events, with the goal of helping to improve patient care, potentially reducing errors and possibly leading to better experiences and outcomes for patients and staff.
Find out more about Philips Capsule Alarm Insights Manager and Clinical Insights Manager.
Jennifer Rist is a Senior Product Manager for Clinical Analytics at Philips Capsule.
Youssef Abou-Hawili is a Fellow Architect Leader for Hospital Patient Monitoring Research & Development at Philips.
Learn more about Alarm Insights Manager and Clinical Insights Manager.
Download